Designing a new tool for women's pain relief
Lauren Carlberg (née Kass), PhD
Poppi Biotherapies is working with experts at NC TraCS on a potential new therapy for vestibulodynia.
Up to 16 percent of women will, at some point in their lives, suffer from a condition that many people have never heard of.
The condition, called vestibulodynia, causes ongoing pain in the vulvar vestibule, the tissue surrounding the entrance to the vagina. This pain is often triggered by pressure or touch. Some people experience pain while inserting a tampon, while having sexual intercourse, wearing tighter-fitting clothing, or even sitting down for a long time.
"Women have had to reorganize how to do their jobs or quit their jobs because they can't sit down for long periods of time, or they can't go on road trips because they can't sit in the car for a long period of time," says Lauren Carlberg, a post-doctoral research associate at the UNC Eshelman School of Pharmacy.
Carlberg is contributing to the science being developed by Poppi Biotherapies, a UNC-affiliated startup that wants to help these women. The group is collaborating with FastTraCS, the medical technology incubator at the North Carolina Translational and Clinicals Sciences (NC TraCS) Institute, to develop a device that can deliver pain relief directly to the painful tissue.
"Innovation in the women's sexual health field is important, because these patients have suffered for a long time without having therapies, devices, or technologies specifically made for them."
"Innovation in the women's sexual health field is important, because these patients have suffered for a long time without having therapies, devices, or technologies specifically made for them," Carlberg says.
Different people may develop vestibulodynia for different reasons, and clinicians are not always able to determine the exact cause of a patient's pain. Possible factors include pelvic floor muscle dysfunction, physical or psychological trauma, hormonal changes, increased nerve sensitivity in the vestibular tissue, and inflammatory conditions.
"There's a lot of trial-and-error that goes into seeing what the patient responds to, and then, by process of elimination, determining what might treat the pain," Carlberg says.
First-line treatment for patients includes pelvic floor physical therapy or topical creams, often with local anesthetics or hormones. Providers also sometimes prescribe systemic medications such as gabapentin or anti-depressants, which can have side effects such as dizziness, fatigue, and weight gain. In severe cases, a surgeon can perform a vestibulectomy to remove the painful tissue, but that comes with the inherent risks of any surgery.
One of the most common treatments is lidocaine, a widely available anesthetic that blocks nerve signals where it's applied. Lidocaine creams can help many patients ease their pain, but they also have drawbacks. For one, Carlberg notes, some formulas are designed for thicker skin rather than the tissue near the vagina, so they may irritate sensitive tissue. These creams can also be messy and may spread to other areas unintentionally.
Erin Carey, MD, MSCR
A few years ago, Erin Carey, a gynecologic surgeon at UNC, had an idea for how to overcome some of those issues. Instead of a cream, she wondered if lidocaine could be delivered on a thin medicated film placed directly on the painful area. The film could have a pre-determined dose, preventing patients from over- or under-medicating themselves, and be shaped to fit the vestibule, helping to cleanly apply the medication only where it's needed.
Initially, Carey and some colleagues developed a lidocaine-coated film that patients could apply and then remove after the medication had been delivered. But after conducting some patient feedback and customer discovery, the research team recognized that patients preferred a completely dissolvable film, eliminating the need to remove anything later.
Carlberg joined the team around this time. She completed her PhD at UNC under Shawn Hingtgen, a researcher at the Eshelman School of Pharmacy, and stayed on in Hingtgen's lab as a post-doc. Carlberg focuses her research on drug delivery mechanisms, and she works with clinicians to develop products that can help their patients. She says she liked that Carey knew what her patients needed and wanted her help bringing that idea to life.
"Erin is just super, super passionate, and makes it very easy to get invested and passionate about what these patients are going through," Carlberg says.
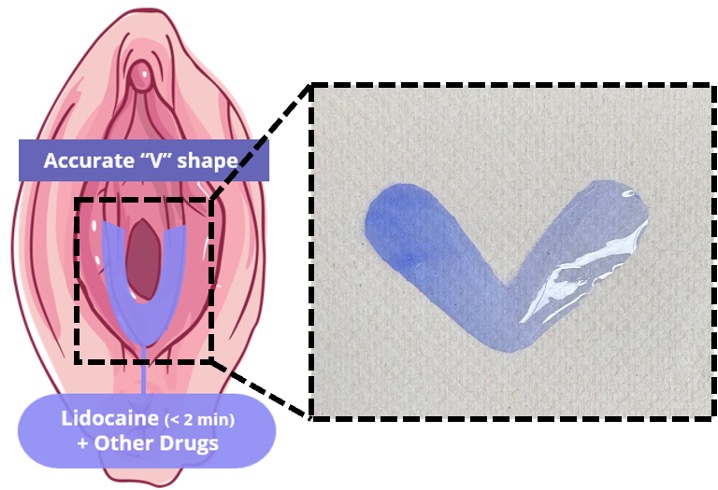
Carlberg and her colleagues developed a new lidocaine-coated film made of a water-attracting polymer that dissolves quickly after it comes into contact with the vestibule. In theory, this new design could simplify the process of using the film.
But the new design also brought on a new challenge. Since the film immediately starts to dissolve after touching tissue, it's difficult to apply by hand. To solve that problem, the team turned to FastTraCS.
The FastTraCS team (including Carey, who serves as co-executive director) helps researchers turn ideas for medical devices and technologies into commercial products. Two of the FastTraCS design engineers, Paula León and Nicole Wiley, are drawing up possible designs for an applicator device that would allow patients to place the film without touching it, based on clinical and scientific team feedback. This applicator device needs to keep the film intact, apply it in the proper position, and work for people with different body types. It also needs to be reusable, so patients could buy it once and then add in film refills.
The team is currently developing three possible prototypes—one larger design with a sliding mechanism to apply the film accurately, one more compact design that could be easily carried around in a bag, and a very compact, fingertip-style applicator. The plan is to 3D-print these designs and then collect feedback from patients.
"Nicole and Paula have been just super creative, and are so talented at what they do," Carlberg says. "They've been amazing at helping us visualize what these things could look like."
Poppi Biotherapies' work has also been supported by the North Carolina Biotechnology Center, which provided them a Flash Grant last year for some initial film development and then a larger Translational Research Grant to help move these devices toward the market.
Soon, this product could help patients achieve more targeted pain relief without the messiness and awkwardness of traditional cream therapies. Since lidocaine is well-studied, the team hopes that the initial approval process for the film and applicator would include lidocaine as an early drug to harness pre-existing safety data and shorten the approval timeline. Eventually, Carlberg notes, other drugs could also be delivered through these films and applicators, especially as researchers learn more about how to support patients with this common, but still largely undiscussed, condition.
"I think this is something that will help people across the country and the world who suffer from vestibulodynia," Carlberg says. "So hopefully we can start that by driving innovation here in North Carolina."
NC TraCS is the integrated hub of the NIH Clinical and Translational Science Awards (CTSA) Program at the University of North Carolina at Chapel Hill that combines the research strengths, resources, and opportunities of the UNC-Chapel Hill campus with partner institutions North Carolina State University in Raleigh and North Carolina Agricultural and Technical State University in Greensboro.

